Plantar fasciitis is one of the most common causes of heel and foot pain, affecting millions of people each year. Whether you’re an athlete, a busy professional on your feet all day, or someone experiencing sudden heel pain for the first time, understanding this condition is the first step toward finding relief. In this guide, we’ll walk through the symptoms, causes, treatments, and prevention strategies to help you get back on your feet comfortably and confidently. Plantar Fasciitis 101: Symptoms, Causes, and Treatments That Work
Plantar fasciitis is the inflammation or irritation of the plantar fascia, a strong band of tissue that runs along the bottom of your foot—from your heel to your toes. This tissue acts as a shock absorber and supports the arch of your foot. When it becomes overstressed or damaged, it leads to sharp, persistent pain that can disrupt your daily routine.
One of the most recognizable symptoms is **intense heel pain during your first steps in the morning**. After periods of rest, the plantar fascia tightens, and when you stand up, the sudden stretching triggers sharp discomfort.
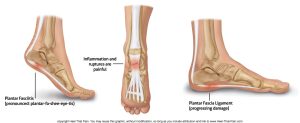
You may notice that your heel hurts after sitting for long periods, driving, or watching TV. This stop-and-start pattern is a classic sign of plantar fasciitis.
While activity can temporarily loosen the fascia and reduce pain, discomfort often returns shortly after you stop exercising. This delayed pain distinguishes plantar fasciitis from other athletic injuries.
Some individuals experience **tightness or stiffness in the arch**, especially when flexing the foot or stretching the toes.
Activities that place repeated stress on the heel—such as running, walking long distances, dancing, or working on hard surfaces—are major contributors. Over time, the fascia becomes irritated and inflamed.
Shoes with **little arch support, thin soles, or poor cushioning** can increase strain on the plantar fascia. Flat shoes like flip-flops or worn-out sneakers are often culprits.
Individuals with very **high arches** or **flat feet** are more prone to plantar fasciitis because their natural foot mechanics place added pressure on the fascia.
Occupations that require long hours on your feet—such as retail, teaching, warehouse work, or nursing—can contribute to chronic heel pain if proper support is lacking.
When the muscles behind the lower leg are tight, they restrict proper foot movement and increase strain on the heel and arch.
Excess body weight increases pressure on the plantar fascia with every step, making inflammation more likely.
The first step toward healing is giving your feet a break. Reduce high-impact activities like running or jumping and switch to low-impact exercises such as swimming or cycling while your foot heals.
Applying ice helps reduce inflammation and pain. Roll your foot over a frozen water bottle for 10–15 minutes twice a day. This method allows both icing and gentle stretching.
Stretches are among the most effective treatments for plantar fasciitis.
Key stretches include:
Calf stretches against a wall
Towel stretches, pulling your toes toward you
Plantar fascia stretch, rolling your foot over a tennis or massage ball
Consistent stretching reduces tightness and promotes long-term relief.
Investing in shoes with **excellent arch support and cushioned heels** can dramatically reduce symptoms. Look for orthopedic-friendly options or visit a specialty store for proper fitting.
Custom or over-the-counter orthotics redistribute pressure across your foot and support your arch. They are especially beneficial for people with flat feet or high arches.
A physical therapist can guide you through strengthening and mobility exercises designed to support foot mechanics and reduce inflammation. Treatment may also include massage, taping, and manual adjustments.
Medications like ibuprofen or naproxen can reduce pain and swelling. They are best used in combination with other treatments, not as a standalone solution.
Night splints hold your foot in a gently stretched position while you sleep. This prevents the plantar fascia from tightening overnight, reducing that painful morning step.
Extracorporeal shockwave therapy (ESWT) uses sound waves to stimulate healing in chronic cases. It’s non-invasive and often recommended if traditional treatments don’t work.
In severe or persistent cases, a doctor may recommend a corticosteroid injection to reduce inflammation. These can provide short-term relief but should not be overused.
Surgery is only considered when all other treatments fail after 6–12 months. The procedure involves releasing tension in the plantar fascia but comes with potential risks and recovery time.
Make supportive shoes your everyday choice—even around the house. Avoid flat, unsupportive shoes that strain your arch.
Daily calf and foot stretches help maintain flexibility and prevent the fascia from becoming tight and irritated again.
Maintaining a healthy weight reduces pressure on your feet and lowers the risk of reinjury.
Running shoes typically lose support after 300–500 miles. Replace footwear regularly to maintain proper cushioning.
A proper warm-up improves mobility, reduces strain on the fascia, and supports healthier foot mechanics.
If your heel pain persists for more than six weeks, becomes severe, or interferes with daily activities, it’s time to see a healthcare professional. A podiatrist or orthopedic specialist can perform an evaluation, recommend custom treatment options, and rule out other conditions such as stress fractures or tendon issues.
Plantar fasciitis is painful, but with the right approach, it’s entirely treatable. By understanding its symptoms, identifying the causes, and using effective treatment strategies, you can significantly reduce pain and prevent future flare-ups. Consistency is key—small daily habits like stretching, wearing proper shoes, and managing activity levels can make all the difference.