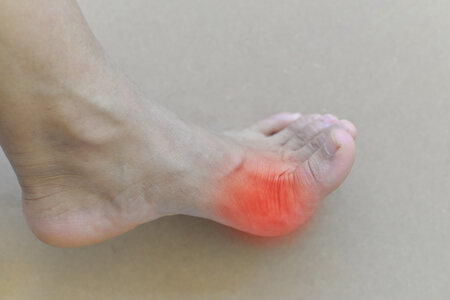
Metatarsalgia is a common but often misunderstood condition that causes pain and inflammation in the ball of the foot. Whether the discomfort comes from intense exercise, improper footwear, or natural foot structure, metatarsalgia can significantly affect your ability to walk, run, or stand comfortably. This comprehensive guide explains the symptoms, causes, treatments, and preventive strategies so you can better manage and overcome this frustrating condition.
Metatarsalgia refers to pain and swelling in the metatarsal region—the area just behind your toes. The metatarsal bones carry a significant amount of your body weight during movement, so when they experience excess stress, irritation and inflammation can develop. While the condition isn’t usually serious, the pain can be sharp, chronic, and disruptive if left untreated.
The most characteristic symptom is **sharp, aching, or burning pain** in the ball of the foot. This discomfort may worsen during standing, walking, or running and often improves with rest.
Some individuals experience tingling, numbness, or a sensation similar to having a pebble in their shoe. This occurs when irritated metatarsal nerves become compressed.
High-impact activities such as jumping, sprinting, or climbing stairs can intensify the pain. People often notice the discomfort increases the longer they stay on their feet.
Rest frequently reduces discomfort. However, untreated metatarsalgia can worsen over time, making pain more persistent and less responsive to rest.
Athletes—especially runners—are prone to metatarsalgia due to repeated pressure on the metatarsal bones. Hard training surfaces, poor running form, and long distances can contribute to chronic strain.
Shoes with **thin soles, high heels, or insufficient arch support** place excessive pressure on the ball of the foot. High heels shift weight forward, while poorly cushioned shoes fail to absorb impact.
Your natural foot structure plays a major role in how pressure is distributed across your foot. – **High arches** may create concentrated pressure on the metatarsals. – **Flat feet** can lead to overpronation, increasing strain on the forefoot.
Individuals with **Morton’s toe**—where the second toe is longer than the big toe—often experience more pressure on the second metatarsal head, increasing the risk of inflammation and pain.
Being overweight or experiencing sudden weight gain increases the load on the forefoot, creating more stress and irritation.
As we age, the natural fat pad that cushions the ball of the foot becomes thinner. This loss of cushioning makes the metatarsal bones more vulnerable to irritation.
Previous foot injuries, fractures, or conditions like bunions and hammertoes can alter alignment and redistribute weight in ways that overstress the metatarsals.
One of the simplest but most effective treatments is taking time off from high-impact activities. Allowing the foot to heal reduces inflammation and pain.
Applying ice to the painful area for 15–20 minutes a few times a day helps reduce swelling and numb discomfort. Use an ice pack or bag of frozen peas wrapped in a towel.
Wearing shoes with: – **Cushioned soles** – **Proper arch support** – **Wide toe boxes** can significantly reduce metatarsal pressure. Avoid high heels and overly flexible shoes during recovery.
Orthotics—either custom-made or over-the-counter—help redistribute weight away from the metatarsal heads. Metatarsal pads, placed behind the ball of the foot, can provide targeted relief.
Strengthening the foot and improving flexibility relieve strain on the metatarsals. Effective exercises include: – **Calf stretches** to improve ankle mobility – **Toe curls and towel scrunches** to strengthen foot muscles – **Arch lifts** to support foot structure
Regular stretching also reduces the risk of future flare-ups.
NSAIDs such as ibuprofen can temporarily reduce inflammation and pain. These should be used cautiously and in combination with physical treatments.
Maintaining a healthy body weight reduces pressure on the forefoot and improves long-term foot health.
A physical therapist can evaluate your gait, foot mechanics, and strength to create a personalized treatment plan. Techniques may include massage, manual adjustments, taping, and customized exercises.
For persistent cases, **extracorporeal shockwave therapy** stimulates healing in damaged tissues. It is non-invasive and typically reserved for symptoms that don’t respond to standard treatment.
Surgery is rarely needed but may be recommended if structural issues, bone misalignment, or chronic nerve compression are present. Procedures can include shortening long metatarsal bones or correcting deformities.
Wear shoes with excellent cushioning, sturdy soles, and supportive arches. Replace worn-out shoes regularly, especially if you are active or walk long distances.
Orthotic inserts help maintain proper foot alignment and reduce stress on metatarsal heads. Using them in everyday shoes—not just athletic ones—can greatly reduce pain.
Keeping your weight within a healthy range prevents excessive pressure on the forefoot.
Regular foot-strengthening exercises improve stability and distribute pressure more evenly across the foot.
If you begin to feel discomfort in the ball of your foot, address it early. Resting or modifying activity at the first sign of pain can prevent chronic issues.
If your foot pain persists longer than a few weeks, worsens with activity, or is accompanied by swelling or numbness, consider consulting a podiatrist. They can perform imaging tests, evaluate your foot structure, and recommend targeted treatment options.
Metatarsalgia can be painful and frustrating, but with the right knowledge and treatment plan, relief is more than achievable. Understanding the causes, identifying symptoms early, and adopting preventative habits can help you stay active while protecting the health of your feet. With supportive footwear, proper stretching, and mindful foot care, you can reduce pain, restore comfort, and move with confidence again.