Flat feet—also known as fallen arches—are extremely common and can affect people of all ages. For some, flat feet cause no issues at all. For others, they can lead to chronic foot pain, balance problems, and discomfort that makes walking or standing difficult. Understanding what flat feet are, why they develop, and how to treat the resulting pain can help you stay active, improve comfort, and protect your long-term foot health. In this comprehensive guide, you’ll learn everything you need to know about flat feet and foot pain, including causes, symptoms, effective treatments, and prevention tips.
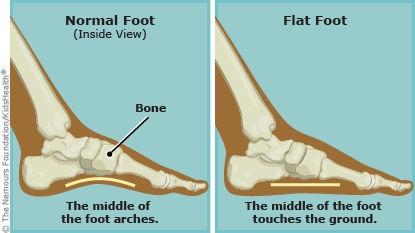
Flat feet occur when the arches of the feet collapse or fail to develop properly. Instead of having a noticeable curve, the entire sole touches the ground when standing. There are two main types of flat feet:
This is the most common type, where the arch appears when the foot is lifted but flattens when weight is applied. It typically develops during childhood and continues into adulthood.
With rigid flat feet, the arch does not appear whether the foot is bearing weight or lifted. This type is less common and may be linked to structural issues, injuries, or medical conditions.
Arch fatigue, heel pain, or general aching in the bottom of the foot are common symptoms. Many individuals experience pain after long periods of standing or walking.
Flat feet can alter the alignment of your lower legs, causing strain on the ankles, calves, and knees. Over time, this misalignment can create chronic discomfort.
Inflammation or swelling near the arch or inner ankle is a typical sign of flat feet, especially if the posterior tibial tendon is involved.
Because flat feet reduce natural shock absorption, your feet may tire quickly, particularly during high-impact activities or long work shifts.
Many people with flat feet overpronate, meaning their ankles roll inward as they walk. Overpronation can affect gait and increase the risk of additional injuries.
Flat feet often run in families. If one or both parents have fallen arches, their children are more likely to develop the same condition.
The posterior tibial tendon plays a crucial role in supporting the arch. When this tendon becomes weakened or injured, the arch can collapse.
As we get older, the tendons and ligaments in the feet naturally lose strength and elasticity, which can contribute to fallen arches later in life.
Excess body weight increases pressure on the feet, making the tendons work harder to maintain the arch. Over time, this pressure can lead to flat feet and pain.
Sprains, fractures, and long-term wear and tear can change the structure of the foot, resulting in fallen arches.
Certain health conditions—such as cerebral palsy, diabetes-related neuropathy, or muscular dystrophy—can affect foot structure and arch support.
With little or no arch to absorb shock, muscles in the feet work harder to stabilize movements, leading to soreness and fatigue.
Flat feet can alter how the ankles, knees, and hips line up during movement, creating pain not just in the feet but throughout the lower body.
Excessive inward rolling of the ankles increases stress on ligaments and bones, contributing to plantar fasciitis, shin splints, and tendonitis.
When the arch collapses, pressure shifts to different areas of the foot, increasing the risk of calluses, bunions, and metatarsalgia.
Wearing shoes designed for stability and arch support is one of the most effective ways to manage flat feet. Look for: – Firm heel counters – Structured arch support – Cushioned midsoles – Wide toe boxes
Avoid flimsy or overly flexible shoes.
Orthotics help correct alignment, support the arch, and relieve pain. Options include: – Over-the-counter arch supports – Custom orthotics made by podiatrists – Metatarsal pads if ball-of-foot pain is present
Orthotics are especially beneficial for overpronation.
Strengthening the muscles that support the arch can reduce pain and improve foot function. Effective exercises include: – Toe curls with a towel – Arch lifts – Heel raises – Short-foot exercises
Doing these regularly can significantly improve stability.
Tight calves and Achilles tendons can worsen flat-foot symptoms. Daily stretching helps improve flexibility and reduces strain.
Maintaining a healthy weight reduces pressure on the arches and can prevent worsening of symptoms.
For flare-ups, ice packs and NSAIDs can help reduce swelling and relieve pain. These should be used together with supportive treatments.
A physical therapist can evaluate your gait, strengthen weak muscles, and teach proper movement patterns to reduce pain.
In some cases, ankle braces or supportive taping techniques help stabilize the foot and reduce pain during activity.
Surgery is considered only when conservative treatments fail. Procedures may involve tendon reconstruction, bone realignment, or arch stabilization.
Choose supportive shoes even at home. Avoid walking barefoot on hard surfaces if you experience pain.
Once you find inserts that work, use them in all your frequently worn shoes.
Making foot exercises part of your daily routine prevents strain from returning.
Running on hard surfaces or standing for long periods can worsen pain. Opt for lower-impact activities like cycling or swimming when needed.
Shoes lose support over time. Replace them regularly—especially athletic footwear.
If pain persists longer than a few weeks, worsens, or interferes with daily life, a podiatrist can help identify underlying issues. Medical evaluation is especially important if swelling, numbness, or tendon pain is present.
Flat feet are common, but ongoing pain is not something you have to live with. By understanding the causes, symptoms, and treatment options, you can take control of your foot health and reduce discomfort. Whether it’s choosing supportive shoes, using orthotics, strengthening your feet, or seeking professional care, there are many effective solutions available. With the right approach, people with flat feet can walk, run, and live comfortably without constant foot pain.