Heel pain is a widespread problem that affects millions of people worldwide. Whether you are an athlete, a busy professional, or someone who spends long hours on their feet, heel pain can significantly impact your daily activities. Understanding the causes and treatment options is crucial for effective relief. This article explores the most common causes of heel pain and provides actionable strategies to alleviate discomfort and prevent future issues. Heel Pain Relief: How to Treat the Most Common Causes
Heel pain can originate from various conditions, ranging from mild inflammation to chronic structural problems. Identifying the root cause is essential to target the right treatment.
Plantar fasciitis is one of the most prevalent causes of heel pain. It occurs when the plantar fascia—a thick band of tissue connecting your heel bone to your toes—becomes inflamed. Symptoms include:
Sharp pain in the bottom of the heel, especially in the morning
Pain after prolonged standing or physical activity
Tenderness along the arch of the foot
Risk factors include obesity, long periods of standing, wearing unsupportive shoes, and high-impact activities like running.
Achilles tendinitis affects the tendon that connects your calf muscles to the heel bone. Inflammation in this tendon can lead to pain at the back of the heel, stiffness, and swelling. Contributing factors include:
Sudden increase in physical activity
Tight calf muscles
Poor footwear or inappropriate exercise techniques
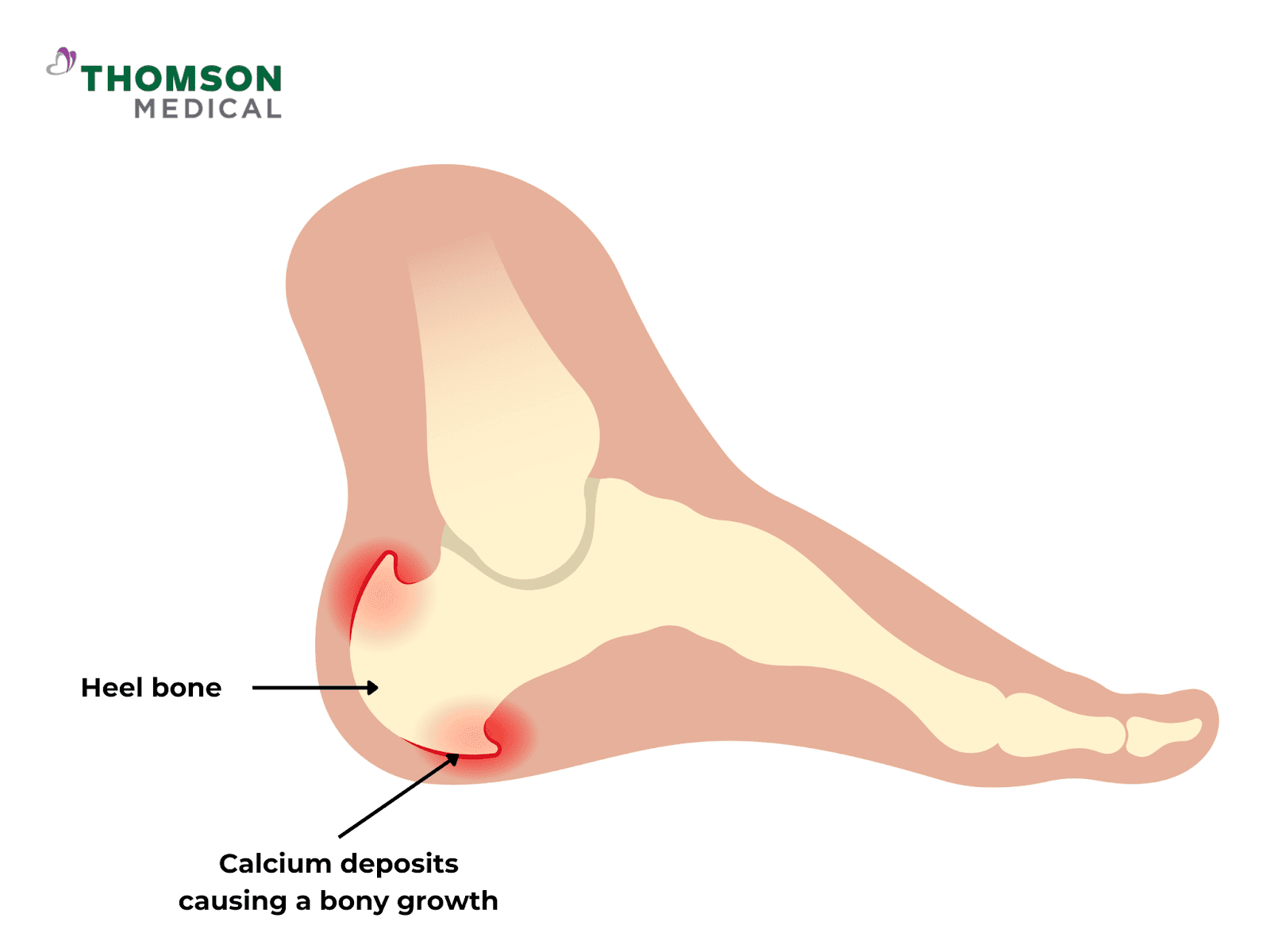
Heel spurs are bony growths that develop on the underside of the heel bone. While they may not always cause pain, they can irritate surrounding tissues, leading to discomfort. Heel spurs are often associated with plantar fasciitis and are detected through X-rays.
Bursitis is inflammation of the bursa—a small fluid-filled sac that cushions bones and tendons. In the heel, retrocalcaneal bursitis can cause swelling, redness, and pain at the back of the heel, especially when walking or wearing tight shoes.
Stress fractures are tiny cracks in the heel bone caused by repetitive stress. Athletes, particularly runners, are at higher risk. Symptoms include:
Sharp, localized heel pain
Swelling and bruising
Pain that worsens with activity and improves with rest
Treatment strategies for heel pain vary depending on the underlying cause. However, some approaches are universally beneficial for reducing inflammation, alleviating pain, and promoting healing.
Reducing or modifying activities that worsen heel pain is critical. This may involve:
Avoiding high-impact sports
Taking breaks from prolonged standing
Using low-impact exercises like swimming or cycling
Rest helps prevent further injury and allows the inflamed tissues to heal.
Stretching exercises improve flexibility in the plantar fascia, Achilles tendon, and calf muscles. Key exercises include:
Calf stretches: Stand facing a wall with one leg behind the other, keeping your back heel on the floor and leaning forward.
Plantar fascia stretch: Sit with one leg crossed over the other, pulling your toes toward your shin.
Towel curls: Place a towel on the floor and use your toes to scrunch it toward you.
Strengthening exercises help prevent future heel injuries by supporting the foot’s arches and improving overall stability.
Wearing proper footwear is crucial for heel pain relief. Look for shoes with:
Adequate arch support
Cushioned heels
Proper fit without pressure points
Custom or over-the-counter orthotic inserts can help redistribute pressure and support the foot’s natural structure, reducing strain on the plantar fascia and Achilles tendon.
Applying ice to the affected heel for 15–20 minutes several times a day can reduce inflammation and relieve pain. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen may also help manage pain and swelling.
A licensed physical therapist can design a personalized program to target your heel pain. Therapy may include:
Manual therapy to improve tissue mobility
Ultrasound or laser therapy for pain reduction
Guided stretching and strengthening routines
For severe heel pain, a doctor may recommend corticosteroid injections. These injections reduce inflammation and provide temporary pain relief, often allowing patients to participate more comfortably in physical therapy.
Surgery is generally considered a last resort, reserved for chronic heel pain that does not respond to conservative treatments. Procedures may include:
Plantar fascia release
Removal of heel spurs
Repair of torn tendons
Surgical recovery requires careful rehabilitation and may take several months.
Preventing heel pain is just as important as treatment. Some effective strategies include:
Excess weight places extra stress on the heels and can contribute to plantar fasciitis and other foot problems. Maintaining a healthy weight reduces strain and promotes overall foot health.
Always choose shoes appropriate for your activities. Avoid worn-out shoes, high heels, and footwear with minimal support.
Incorporate daily foot and calf stretches to maintain flexibility and prevent tendon or fascia injuries. Strengthening exercises can improve foot stability and reduce the risk of future pain.
Whether starting a new exercise program or returning from injury, gradually increase intensity and duration. This approach minimizes stress on the heel and allows tissues to adapt safely.
Most heel pain can be managed at home with rest, ice, and stretching. However, consult a healthcare professional if you experience:
Severe or worsening pain
Swelling, redness, or warmth around the heel
Pain that does not improve with conservative treatment
Numbness or tingling in the foot
Early intervention can prevent chronic conditions and ensure a faster recovery. Heel Pain Relief: How to Treat the Most Common Causes
Heel pain is a common yet manageable condition. By understanding its causes—from plantar fasciitis to Achilles tendinitis—and implementing targeted treatments like stretching, proper footwear, and physical therapy, you can find relief and restore mobility. Prevention through healthy habits and gradual activity adjustments is key to avoiding future discomfort. With the right approach, most people can recover fully and enjoy an active, pain-free lifestyle.